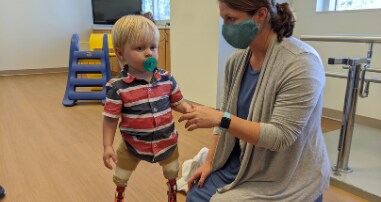
When you choose the Comprehensive Limb Difference Program at Children’s Healthcare of Atlanta, you are choosing unmatched expertise and care. Backed by decades of experience, our multidisciplinary team provides comprehensive evaluation, surgical intervention, cutting-edge prosthetic and orthotic devices, and tailored therapy for children, teens and young adults with limb differences. Whether congenital or acquired, early intervention is crucial, and we prioritize meeting the evolving functional needs of our young patients, as well as their emotional well-being. If your child needs to stay in the hospital after their surgery, we offer support from child life specialists to provide holistic care for patients as well as their families. Trust the experts at Children’s for compassionate care and unwavering dedication to improving the lives of those with limb differences.
Limb differences can include deficiencies, deformities or discrepancies that make a limb appear different.
Limb deficiency
A limb deficiency is when a child’s leg, arm, hand, finger, foot or toe is crooked, uneven, partially formed or even missing. It can affect the whole limb or just part of the limb and can be congenital (present at birth) or acquired (the result of a disease, accident or other trauma).
Limb deformity
A limb deformity is a misshapen limb. A deformity can affect the appearance and function of upper limbs like the arms, hands and fingers, as well as lower limbs like the legs, feet and toes.
Limb length discrepancy
If a child has a limb length discrepancy, which means the limbs are uneven, it may be caused by limb deficiency problems or complications from broken bone growth plates and may be the result of:
- Failure of formation.
- Abnormal formation.
- Too many bones and fingers.
- Too few bones and fingers.
What causes congenital limb differences in children?
The cause for most limb deficiencies, deformities and discrepancies is unknown, but it’s assumed that amniotic bands could be a cause of limb deficiency in upper or lower limbs. Others may be inherited, although this is rare. For some limb differences, however, there may be underlying bone problems like rickets, which can lead to bent bones, or osteogenesis imperfecta (brittle bone disease), that can lead to deformities from multiple fractures.
Simply stated, a child's limb difference or deficiency can be the result of:
- Lack of formation in utero.
- Abnormal formation in utero.
- Too many bones and fingers forming in utero.
- Too few bones and fingers forming in utero.
- Amniotic bands tightening around limbs, restricting growth.
- Fractures.
No matter the cause, children with limb differences are all unique, which means their treatment should be individualized to meet the needs of each child and family.
Our team created a private Facebook groups for limb deficiency families.
This Facebook page offers an online resource for sharing advice, seeking recommendations, celebrating milestones (of all sizes!) and getting to know each other.
Learn MoreWe treat babies, kids and teens who are affected by congenital conditions that cause limb deficiencies, deformities and discrepancies. Typically, congenital limb difference is not genetic, but some types of congenital limb difference are hereditary. Depending on the age and goals of a patient and family, a prosthesis can also be worn. These conditions can affect the entire upper and lower parts of the limbs, or just parts of those limbs, including:
Shoulder and arm
- Above the elbow: This is an arm difference that occurs during development in the womb in which a portion of a child’s arm above the elbow does not develop properly. This can occur immediately above the area where the elbow may be or higher up the arm and typically involves only one arm.
- Below the elbow: This is an arm difference that occurs during development in the womb in which a portion of a child’s arm below the elbow does not develop properly. This can occur anywhere along the length of the forearm and typically involves only one arm.
Forearm
- Radial deficiency: There are two bones that make up the forearm. When all or a portion of the radius (the bone on the thumb side of the forearm) is missing, this can be due to a condition known as radial longitudinal deficiency. When this condition is present, there may also be a spectrum of problems with the thumb, ranging from a normally functioning to an absent thumb. This can sometimes occur spontaneously, but it often is associated with syndromes like thrombocytopenia absent radius (TAR); Holt-Oram; TBX5 deficiency; vertebral defects, anal atresia, cardiac defects, tracheoesophageal fistula, renal anomalies and limb abnormalities (VACTERL); or Fanconi’s. Surgery is often performed to improve overall alignment of the wrist. If other differences exist, such as with the thumb, surgery can be performed in order to help its function or create a finger to work like a thumb.
- Ulna deficiency: When all or a portion of the ulna (the bone on the small finger side of the forearm) is missing, this can be due to a condition known as ulnar longitudinal deficiency. Small and ring fingers may also not develop. This condition occurs occasionally, and surgery may sometimes be performed to improve the position of the wrist and forearm.
Hand and Fingers
Differences of the fingers, or digits, and hands happen when a portion or all of a finger, fingers or hand did not develop or form properly in the womb. Specific conditions that can affect the hand and fingers include:
- Amniotic band: This condition occurs when a baby is born with multiple band-like wrappings around the arms. This can result in amputated fingers, connected fingers (syndactyly) or nerve dysfunction depending on where the band-like wrappings around the arms are located. The cause is unknown, and it happens occasionally.
- Camptodactyly: This occurs when a finger is unable to be straightened out. It most commonly occurs in the pinky. It is a spontaneous condition but can be genetic. Management is commonly conservative, with stretching and splinting as directed by therapy. When shortening of the muscle or bone is severe, surgery is occasionally performed to help straighten the finger.
- Cleft hand: Children may be born with a widened space between their fingers or missing middle fingers. This condition is known as cleft hand. This is typically a genetic condition, but it can occur spontaneously. Some children may function well with grasp and may not need surgery to improve this function. When treated surgically, reconstruction can be performed to narrow the webbed space between the fingers. Children may have the same deformity in their feet, which may require special shoes or orthotic management.
- Cleft hand, atypical symbrachydactyly: This is a condition in which the hand may be smaller than normal, and the fingers may not fully form and be interconnected. The fingers can vary in length and function. The thumb is usually spared, and typically only one hand is involved. This occurs spontaneously or in association with Poland syndrome. Surgery can sometimes be performed to help the hand pinch better. Examples of surgery may include deepening the thumb’s webbed space, finger lengthening or a toe-to-finger transfer. Surgery varies from hand to hand. Prostheses may be helpful for certain activities on a patient-specific basis.
- Clinodactyly: This is when just the tip of a finger is curved, typically in the direction pointing toward the thumb. This can occur spontaneously, genetically or in association with Down syndrome. The finger typically functions very well. Surgery may be considered for fingers that overlap when trying to grip.
- Kirner: This is when the tip of the finger has a more curved appearance than other fingers. It is a spontaneous condition but can be genetic. These fingers typically function very well. Surgical intervention may be warranted if the shape of the finger impedes function.
- Syndactyly: This is a condition in which two or more fingers are stuck together, have no webbed space and are incapable of being separated. Fingers often remain attached by skin only, but sometimes the bones, nerves and blood vessels can be involved between two fingers. The cause of this condition can be spontaneous, genetic or occur with other conditions. In most circumstances, surgery can be performed to separate the fingers. There is usually not enough skin to split the fingers, so skin is typically taken from somewhere else on the body to help cover the deficit. When bones are involved, separating fingers may compromise the function of the hand.
- Amniotic band: This condition occurs when a baby is born with multiple band-like wrappings around the legs, feet or toes. The cause is unknown, and it happens occasionally.
- Longitudinal deficiency of the femur (congenital femoral deficiency, or CFD; or proximal femoral focal deficiency, or PFFD): This condition involves the femur (thigh bone), hip joint above the femur, knee joint below the femur and muscles that cross the hip joint. The main feature of this disorder is that the femur bone is too short. In most children, not only is the femur severely shortened, but the hip joint is also deformed. In some cases, a hip joint may not form at all. Longitudinal deficiency of the femur may be associated with other limb deficiency conditions, with the most common one being a longitudinal deficiency of the fibula.
- Longitudinal deficiency of the fibula (fibula deficiency or fibular hemimelia): A birth defect in which part or all of the fibula is missing or shortened.
- Longitudinal deficiency of the tibia (tibia deficiency, tibia hemimelia): This is a rare congenital deficiency (reported in 1 in 1 million children) that involves the tibia (shin bone). It can vary from a mild amount of shortening to absence of the bone. The knee and ankle joints tend to be affected to some degree. Some forms of longitudinal deficiency of the tibia are inherited, while others occur with no apparent cause. Oftentimes (approximately 50%), tibia deficiencies can be associated with other conditions, such as congenital femoral deficiency, an absent patella (kneecap) or clubfoot. In approximately 30% of cases, longitudinal deficiency of the tibia is bilateral (in both legs). The presence or absence of a tibia and how short the limb is projected to be, as well as the functionality of the knee and ankle joints, help determine treatment options. The goal is to maximize function and have the limbs be close in length by the time the child reaches adulthood. Surgery to remove the affected tibia and fibula, amputation or limb lengthening procedures are options to correct the deformities. A prosthesis may be required after amputation.
- Clubfoot (congenital talipes equinovarus, or CTEV): This is a deformity of the foot present from birth.
- Cleft feet or ectrodactyly (split hands and feet malformations): Like cleft hand deformity, cleft feet deformity effects the toes and bones in the center of the foot creating a large space in the middle of the feet.
- Syndactyly: Webbing of the toes.

National and international research is a top priority for Children’s
Our comprehensive limb difference team wants to provide better outcomes for limb difference patients through collaboration and research.
Learn moreSome limb differences may be acquired, which means they develop over time or happen because of an injury, such as a fracture, accident, infection, tumor or condition effecting the bone’s formation and growth.
Post-traumatic limb deformity (fracture)
A post-traumatic limb deformity is a limb that becomes crooked after a bone is broken. In some cases, the bone may heal in a crooked position, which is known as a fracture malunion. Other times, the fracture may heal straight, but the bone’s growth plate is partially damaged. This causes the bone to heal crooked or grow at a different length than the opposite limb.
In children, fracture malunions are often not a problem if the crookedness is not causing any pain or the child can still use the limb normally. This usually happens if the fracture is close to the growth plate but does not affect the growth plate. Infections may also affect a bone’s growth plate.
If your child has recently had a fracture or infection involving the growth plate, your doctor will follow the growth of your child’s limb for at least six to 12 months to determine whether there are any problems. Some types of deformities do not need treatment and get better over time. In some children, a crooked bone will not improve its alignment as it grows, and it will become painful or cause functional problems. If this is the case, your child’s doctor can talk to you about options to straighten the bone.
Post-traumatic limb deficiency (amputation)
Our team of specialists understands how to deal with traumatic events that may require amputation, rehabilitation and follow-up care. Acquired amputations happen most often as a result of trauma, infection or bone tumor. The majority of amputations happen because of trauma. Our team offers a multidisciplinary approach to caring for children, teens and young adults who need a limb amputated.
Tumors and infections
Some infections may require amputation so that the disease does not spread. Tumors and sarcomas can also result in the need to have surgery on or amputate a limb.
Some types of tumors that may require amputation include osteosarcoma, Ewing’s sarcoma and rhabdomyosarcoma. Your child’s care team will work to understand the type of treatment that will be best in his case. Determining whether a limb can be saved depends on how aggressive the tumor is, the stage of the tumor, how effective other medical treatments have been and whether there is a good chance the surgeon can remove all of the tumor.
If surgery is determined to be the best approach for treatment, our team offers a range of treatment options as part of our Bone and Soft Tissue Sarcoma Program.
A New Musculoskeletal Tumor Clinic
Our multidisciplinary Musculoskeletal Tumor Clinic brings together orthopedic surgeons, hematology oncology physicians and physical therapists who are specially trained to treat kids with sarcomas (bone tumors).
Call Us NOwThe Comprehensive Limb Difference Program team at Children’s offers a collaborative approach to limb difference treatments and customizes plans for each patient, including pediatric orthopedic specialists, physical therapists and orthotists to help make sure your child’s limbs remain as functional as possible. Treatment options include:
Our orthotics team creates custom fit braces and splints to help patients with limb deformities and deficiencies including:
- Orthotics
- Splints
- Casts
- Braces (Orthoses)
- Special shoes
Our prosthetists and orthotists are certified by the American Board for Certification (ABC) in Orthotics and Prosthetics and Georgia licensed practitioners who are specially trained to work with children.
Prostheses and assistive devices, including custom 3D- printed devices, are designed to meet the functional demands and needs of children with upper and lower limb loss. There is no right or wrong decision when it comes to whether a child should wear a prosthesis or use an assistive device.
There are many options for lower and upper limb prostheses. Understanding the types of prostheses available for the level of limb loss helps a child and family make the decision that is right for them. The decision for the best type of prosthesis or assistive device for your child is made by your child’s team that includes your child, family, community therapists and teachers when appropriate, and doctors. Your child’s team will provide prostheses that are thoughtfully and carefully designed to meet the needs of each individual child to help ensure the physical needs of a child are met to allow the greatest function in their environment. At Children’s, we specialize in designing durable prostheses that can withstand the demands of active growing children. We are able to design prostheses to accommodate all shapes at any stage of your child’s growth and development. Our goal is to enable children to participate fully and confidently in their communities no matter their age or degree of the limb difference.
Lower limb prosthesis
- Partial foot prosthesis: These prostheses provide support for a missing part of a foot to allow for a more normal gait and can range from a silicone prosthesis to a shoe filler or AFO.
- Syme or below-the-knee prosthesis: This type of prosthesis consists of a socket and foot or ankle component. Feet may be made of different materials, including carbon and fiberglass composites. There are many feet on the market to choose from, so the prosthetist will work with your child closely to determine the specific needs to help ensure optimal outcomes.
- Rotationplasty prosthesis: A rotationplasty prosthesis is designed for a child who has had a rotationplasty surgery for either sarcoma or PFFD. It has a rigid socket with outside joints that provide stability at the ankle, which is acting as the knee, and a leather corset for support. A prosthetic foot is chosen based on a child's activity and lifestyle.
- Above-the-knee prosthesis: An above-the-knee prosthesis will include a socket, knee and foot. The knee of a prosthesis may be single-axis or polycentric, with friction, hydraulic or microprocessor (computer) control. The prosthetic foot compliments the knee to allow for a smooth, stable walk. We believe most children are able to learn to use a functioning knee in their very first prosthesis.
- Hip disarticulation or hemi-pelvectomy prosthesis: This prosthesis incorporates a hip joint, in addition to a prosthetic knee and foot. Our team has experience and expertise in supporting children using this high-level device.
- Extension prostheses: Some conditions like PFFD may require a prosthesis before surgery. The goal is to provide a child with equal leg lengths as they learn to walk, climb and run, and until the time of their surgery to correct the limb deficiency.
- Sports and activity-specific prostheses: These prostheses are designed to help children compete at high levels or for specific activities, such as a snowboarding prosthesis or a rock-climbing prosthesis. Many children use their daily prostheses for most sports until they specialize in a sport in high school. Our therapists are specially trained in teaching children to run with a prosthesis.
Upper limb prosthesis and assistive devices
Upper extremity prostheses include non-articulating functional prostheses, body-powered prostheses, myoelectric prostheses, activity-specific prostheses and custom-made assistive devices that include 3D-printing technology. Our team also offers prosthetic training provided by therapists who are experienced in working with children, teens and young adults during all stages of prosthetic use.
- Non-articulating functional (fingers of the prosthetic hand do not move): These prostheses are generally worn to give children equal arm lengths and help with simple tasks, such as propping for independent sitting, support during tummy time, balance and global strengthening. Non-articulating prostheses can be skin tone matched to the child, incorporating a soft hand for oppositional tasks.
- Body-powered: Body-powered prostheses provide grasp and release functions that operate a prosthetic hand (also called a terminal device) with a cable and harness. A harness is worn around the child’s shoulders so that tension on the cable that is attached to the harness either opens or closes the terminal device: a prosthetic hand, pre-hensor or hook. Body-powered devices are durable, provide excellent proprioceptive feedback and can help a patient improve their fine motor skills.
- Myoelectric: A myoelectric prosthesis is an active, electronically powered device that allows children to open and close a prosthetic hand for grasp and release functions. Small electrodes are built into the socket, which detects signals from the muscles under the electrodes. The signal from the muscle helps control the speed and degree of opening. This technology helps increase independence, while also providing a more natural appearance than many conventional prostheses. As children grow, the ability and appearance of the hand becomes more important to them. This technology is well-suited for teens through adulthood.
- Multi-articulated digits: For older patients, advanced innovative prosthetic devices are available that provide independent movement of each finger, as well as stronger and faster grasp and release functions. These include the I-Limb, Michelangelo, BeBionics, Taska and various other advanced options. Using specially designed computer software, gesture control or even a phone application, patients can program grip patterns and access other hand features. New technology like pattern recognition will make using these advanced devices even easier. We offer two types of multi-articulated digit prostheses: one for full-hand deficiency and another for partial-hand deficiency. Children’s is one of the first providers in Atlanta to offer advanced microprocessor upper extremity prosthetic technology.
- Sports, recreation and activity-specific prostheses: For even the most experienced child who wears an upper extremity prosthesis, there is often a task or sport they find difficult to perform without two hands. These prostheses are designed to help a child perform that specific task or sport. These devices are built with durability in mind to keep the child active while improving the confidence and supporting exploration of various hobbies.
- Silicone restoration: These prostheses are highly cosmetic, real-life stylized, non-articulating functional prostheses. This device provides children who have a partial or complete loss of an extremity—hands, feet, fingers or toes—with a unique and realistic replacement prosthesis. The silicone can be sculpted and painted to match each child’s size and skin tone, including details like wrinkles, veins and freckles. Silicone skins can be made to go over prostheses, including below-the-knee or above-the-knee leg prostheses. As a child grows, a silicone prosthesis can be resized for a consistent appearance. Silicone prostheses require specialized fabrication that takes extra time for the customization.
- Assistive devices: Often, a child may require a “helping hand” to complete a task. These devices aide a child with a specific function, such as holding a spoon or pencil, riding a bike or playing a musical instrument. Every task is important if it has meaning to the child. If a child is having difficulty performing a specific task, the prosthetic team at Children's can customize a simple device or adapt a device. We have 3D-printing technology that is often used to customize these assistive devices.
The rehabilitation team at Children’s is trained and experienced to work with children who are undergoing limb lengthening surgery, limb salvaging procedures or prosthetic training.
- Occupational therapists can help children with physical, mental or cognitive disorders develop, maintain or recover daily living skills.
- Physical therapists can help preserve, enhance or restore movement and range of motion when a disease or injury impairs your child’s ability to move and function physically.
We have advanced treatments for physical therapy, including our specialized pool and aquatics program and our Center for Advanced Technology and Robotics.
The goal of limb lengthening and reconstruction surgery is to correct and realign a limb difference, as well as the gain additional length in the limb. Our surgical team is specially trained to treat children, teens and young adults when limb differences may require surgery.
- Amputation: This is a surgery to remove a limb, either due to a tumor or infection, or to correct a limb deformity when limb reconstruction is not possible. The loss of a limb can be scary, but our pediatric-trained specialists can help children who face this option realize an amputation will only briefly slow them down. Advancements in prosthetic technology have improved patient function and autonomy after surgery. There are also a wide range of adaptive sports and activities available to these patients. To help families make what can be a difficult decision, we connect them with patients and families who have been through the same procedures and recoveries.
- Learn more about congenital amputations
- Learn more about traumatic amputations
- Learn more about pain after amputation
- Limb reconstruction surgery: This is a procedure to realign and shape a bone.
- Limb lengthening surgery: This is a procedure to lengthen or straighten a limb. We have expertise in internal lengthening nails and hexapod external fixator constructs.
- Limb sparing surgery: Also known as limb salvaging, this surgery removes a tumor or sarcoma in a limb without having to remove the whole limb.
- Rotationplasty: This is a limb sparing surgical option for children who have osteosarcoma, or bone cancer, in the femur (thigh bone), knee or tibia (shin bone).
- Straightening: This surgery allows the doctor to straighten the bones.
- Transferring fingers and toes: This surgery is now available in several treatment options for kids who have lost a digit.
- Targeted muscle reinnervation (TMR): This surgery is used to prevent and treat pain, and improve the muscle control for operating an upper limb prosthesis.
The Comprehensive Limb Difference Program at Children’s includes pediatric orthopedic surgeons, as well as pediatric physical therapists, prosthetists and orthotists to help make sure your child’s limbs remain as functional as possible.
Our surgeons have additional training in limb lengthening and reconstruction and remain active in the limb lengthening and deformity communities. This helps make sure your child receives the most up-to-date and informed treatment possible.
Contact our Comprehensive Limb Difference Program
Phone: 404-785-6353Email: limbdifference@choa.org
Orthopedic surgeons
Contact: 404-255-1933
- Jorge A. Fabregas, MD, Co-Lead, Comprehensive Limb Difference Program
- Jill C. Flanagan, MD, Co-Lead, Comprehensive Limb Difference Program; Medical Director, Osteogenesis Imperfecta Program
- Robert W. Bruce Jr., MD, Medical Director, Neuromuscular Program and Cerebral Palsy Program
- Dell C. McLaughlin, MD, MPH
- Dana Olszewski, MD, MPH, Clinical Site Education Director
- Michael L. Schmitz, MD
Contact: 404-785-KIDS (5437)
Physical therapists
Contact:404-785-5684
- Colleen P. Coulter, PT, DPT, PhD, PCS
- Jill Cannoy DT, DPT, PCS
Contact: 404-785-3229
- Brian Giavedoni, MBA, CP, LP
- Rebecca Hernandez, CPO, LPO
- Richard Welling, MSPO, CPO, LPO
- Brian Emling, PO, LPO
Private practice physicians in our Orthopedics Program
We work closely with private practice physicians in our program to lead research, develop specialized programs and deliver seamless care to patients.
Hand surgeonsContact: 404-785-HAND (4263)
Several of our team members are affiliated with:
- Association of Children’s Prosthetic-Orthotic Clinics (ACPOC)
- Amputee Coalition (AC)
- Limb Lengthening and Reconstruction Society (LLRS)
- Musculoskeletal Tumor Society (MSTS)
- Children’s Oncology Group (COG)
- Pediatric Orthopedic Society of North America (POSNA)
- American Academy of Orthopedic Surgeons (AAOS)
- Academy of Prosthetists and Orthotists

Contact Us 404-785-6353