At the Aflac Cancer and Blood Disorders Center of Children’s Healthcare of Atlanta, over 80 children each year are treated for sickle cell disease through a blood and marrow transplant (BMT). As one of the leading pediatric BMT programs in the U.S., we strive to improve and enhance the quality of life for children and young adults with sickle cell disease by offering a BMT as a possible cure.
Bone marrow is the soft, spongy tissue found in bones that makes red blood cells. Hemoglobin is a protein in red blood cells that helps move oxygen through the body.
Blood stem cells that come from a healthy donor make red blood cells with normal hemoglobin, while a child with sickle cell disease makes hemoglobin S. Hemoglobin S can cause red blood cells to be crescent-shaped (C shaped) allowing them to get stuck in blood vessels and block the flow of blood. This leads to sickle cell disease complications, such as pain crisis, acute chest syndrome (ACS) and stroke.
When a child with sickle cell disease undergoes a BMT, he or she receives healthy bone marrow that produces normal red blood cells.
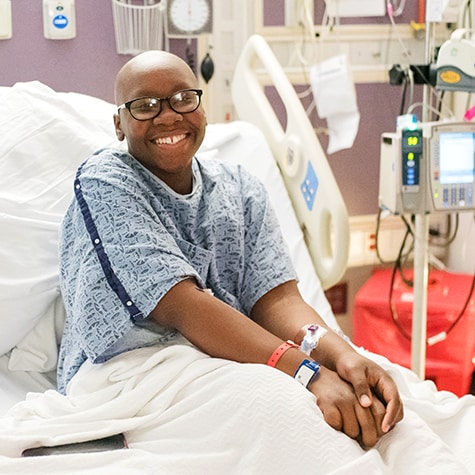
What should I expect if my child needs to have a BMT?
Hear from our experts about what a blood and marrow transplant (BMT) procedure entails so you and your family can feel informed and confident about it.
LEARN MOREBMTs are usually performed on patients with severe sickle cell disease because they are at the highest risk for disability or death as a result of their condition. For a patient who does not have a healthy, matched sibling donor, the risk of BMT complications is higher. Therefore, fewer of these children are candidates for BMTs.
Your child may qualify for a BMT if he has:- Several episodes of ACS
- Stroke
- Severe and/or frequent pain
How is a donor identified?
The best donor is a human leukocyte antigen (HLA)-matched sibling who does not have sickle cell disease. A good match between a donor’s and patient’s HLA markers is essential for a successful BMT outcome. It promotes the growth and development of healthy, new blood cells and reduces the risk of any post-transplant complications.A blood test will be done first on your child’s full siblings (brothers and sisters who have the same parents as your child). They each have a 25 percent chance of matching. If your child does not have a matched sibling, the chance of complications from a BMT is higher.
A donor does not have to be the same blood type or gender as your child to be a match. The donor just needs to have the same HLA type. A donor can also have a sickle cell trait, and the donor’s donated blood stem cells can come from stored cord blood, bone marrow or circulating blood.
How will my child have to prepare for a BMT?
Your child will take medicine to prepare his body for the healthy, new blood stem cells. The medications:- Help his body accept healthy cells during a transplant.
- Can be given to your child in different ways, such as by an intravenous (IV) line or by mouth.
- May cause side effects like nausea, vomiting, hair loss, mouth sores, poor appetite, diarrhea and low blood counts.
How is a BMT performed?
The transplant will be given to your child through his vein using a central venous line (CVL). It can take five minutes or several hours to complete the procedure.What can my child expect after a BMT?
After undergoing a BMT, your child will stay at the hospital for several weeks to be watched closely by his sickle cell disease care team. Your child’s post-procedure care may require him to:- Take many different medicines.
- Follow special rules to prevent infection.
- Stay home from school for a while.
- Need vaccinations or shots to prevent infection.
- Need a full-time caregiver.
- May still pass on the hemoglobin S gene.
What are the risks of a BMT?
The risks of a BMT include:- Rejection of the transplant if your child’s body does not accept the new cells
- Infection
- Infertility
- Stroke or seizure
- Graft-versus-host disease (GVHD) (when the donor’s cells attack your child’s body)
- Death
A BMT is hard on patients and their families because it is such a long process. Our team of professionals performs one of the highest volumes and has some of the greatest outcomes nationwide. We will work to support your family.
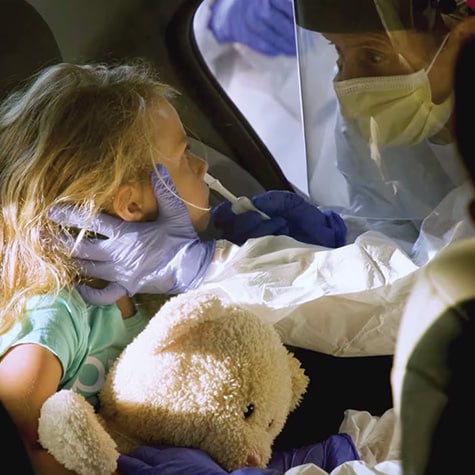
Advancements in treating sickle cell disease are a result of innovative research.
We are committed to improving the quality of life for children with sickle cell disease by offering a BMT as treatment. Our multidisciplinary research team is investigating every aspect of the procedure to help improve outcomes and find innovative treatment options.
FIND A STUDYContact Us 404-785-1200
